Hello! I hope you are well and trying to stay positive about the next month or so… I just wanted to reassure you about the continuity of your ongoing treatment. XPhysio remains remains…  With the announcement over the weekend, I want to update you on our services. As healthcare providers, Physiotherapists are classified as an essential service. XPhysio will remain open as normal. We will continue to follow government guidelines as well as guidelines from Public Health England and our own regulating bodies. Your safety is paramount and we will continue to follow all covid-secure policies in order to remain open. XPhysio will keep you updated with any changes to government policy that affect our services. If you have any questions or concerns regarding any future treatment or upcoming sessions, please do not hesitate in contacting me. See you soon. Emerson XPhysio |
Category Archives: running
XPhysio clinics reopen this week – Monday 18/05/20
XPhysio clinics open from Monday 18th May 2020
Following recently updated guidance (12th May 2020) from NHS England and the Chartered Society of Physiotherapy, we will be offering selective ‘face to face’ appointments from next week. We shall also continue to offer remote consultations.
Any new patients requesting a ‘face to face’ consultation will first receive a brief telephone consultation from one of our clinicians to assess clinical need and screen for any additional risk factors.
Physical appointments will then be offered if deemed clinically appropriate and necessary.
To make an appointment please email info@xphysio.com
After the initial ‘face to face’ consultation, it will be agreed between the patient and therapist whether future treatment sessions can be delivered remotely or if their is a need for ongoing ‘face to face’ sessions.
Our clinic’s locations currently offering ‘face to face’ consultations are Angel N1, Bury Street EC3A (next to the Gherkin) and Dalston E8.

Our 3 Principles for re-opening – Hygiene, Confidence
and Communication
Hygiene – All reasonable infection prevention and control measures are in place and compliant with Public Health England guidelines
Confidence – Patients, staff and the general public can have the confidence of XPhysio’s ongoing commitment to ensuring all safety measures are in place and followed at all times
Communication – XPhysio will be forthcoming with communication to patients, staff and general public at all times – via website updates, blogs, direct communication with all patients booking to attend and on-site information from staff.
The health and safety of our patients and staff are always paramount.
We have been preparing thorough risk assessments for every aspect of our clinic environment and the patient journey to ensure we provide the cleanest and safest environment possible. We have been in contact with industry experts to ensure that our infection prevention and control measures along with PPE (personal protective equipment) not only complies with current guidelines and protocols, but also to minimise any risks of transmission of COVID-19 during treatment sessions. We will continue to follow the guidelines set out by the government and NHS England and respond to any changes to ensure we comply with all the necessary social distancing and personal protective equipment (PPE) protocols .
10 step plan for clinic re-opening
1/ We shall be significantly increasing the level and frequency of cleaning for our clinic sites. Our clinics will be undergoing regular deep cleans to ensure we maintain the highest levels of hygiene within the clinic. Industry recommended virucidal disinfectant cleaning products will be used to minimise the risk of contamination
2/ Face to face appointments will only be offered to patients where effective treatment cannot reasonably be carried out remotely – patients will receive telephone screening consultation
3/ All patients and staff are advised not to attend our clinic if they are displaying possible signs of COVID-19 or if they should be self-isolating under current government guidelines. Patients and staff will be screened before their appointment to ensure they do not have any Covid-19 symptoms
4/ All staff and patients will be temperature checked on entering the clinic and advised not to enter if their temperature > 37.8 Celsius.
5/ Waiting areas and appointment times will be organised to ensure social distancing guidelines can be maintained (2 metres are kept between patients)
6/ Our clinicians will be wearing all the necessary PPE including surgical masks, gloves and aprons at all times during your appointment. If there is any chance of ‘splash back’ from bodily fluids e.g. during exercise, injection therapy, acupuncture or manual therapy, your clinician will wear a visor or eye protection.
7/ We will be operating a significantly reduced service to minimise the number of patients and staff in the clinic at one time
8/ We will be extending our opening hours to spread the flow of patients evenly throughout the day
9/ Between each patient we will allow 15 minutes to deep clean all surfaces using virucidal disinfectant and change the necessary PPE
10/ We can guarantee you these measures will not affect your standard of care
Our aim is to allow patients to attend our clinics with upmost confidence. We are committed to the highest levels of patient care and also transparency in how we operate. If you have any questions or feedback with regards to any of the information above please do not hesitate to contact us. If you would like further information regarding our social distancing measures or PPE guidelines then please do not hesitate in contacting me.
Stay safe.
Emerson
XPhysio
emerson@xphysio.com | 07903 247247
References:
https://www.csp.org.uk/news/coronavirus/clinical-guidance/face-face-or-remote-consultations/guidance-england
https://www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control
Phy-video-therapy?
Physiotherapy and video consultations – New assessments and injury management.

These are very worrying and strange times, for everyone.
I have been agonising over the past week about the options for continuing to offer Physiotherapy services in the current climate.
Ultimately, the combination of collective responsibility, social pressure and doing everything we can to halt the spread of this virus and help out our NHS colleagues on the front line made the decision easy.
During this unprecedented time, we all have had to adapt and find new ways to keep supporting your physical (and mental) health. The world can’t stop and now, more than ever exercise is so important.
I have now moved to all online voice only or video-call sessions via phone, facetime, skype or zoom.us app. This will continue for the short-term (I hope) and we will be able to seamlessly transition back to face-to-face and hands-on when we are able to do so safely.
I have moved all my current patients in treatment seamlessly over to video appointments where possible. But what about new assessments and acute injuries?
What can we accomplish in a new patient online session?
- Face-to-face detailed subjective injury history taking
- Full objective assessment including range of movement, strength tests and special tests
- Diagnosis of the injury
- Advice and anatomical description
- Provide realistic timeframes for management and recovery
- Provide recordable exercise prescription and self-mobility techniques
- Demonstrate taping techniques
- Goal setting for the next session
- Online exercise programming software integration

I am an experienced Physiotherapists and worked in A&E for four years as a musculoskeletal injuries specialist. I still work part-time for the NHS in a Consultant Physiotherapist role, predominantly running Orthopaedic triage clinics which means a lot of very quick assessments and decisions on care! I am also a qualified musculoskeletal Sonographer, Independent prescriber and practice injection therapy.
I thought it might be helpful to give two examples of remote sessions I have been involved with this week.
Case study 1 – 40 year-old fit and actively man was unfortunately stranded in France due to the COVID-19 outbreak. With limited equipment and self-isolating, he took up trail running. After a few runs, he missed a step and felt a sharp pull in the back of his leg. After the pain subsided he hobbled home and used the RICE (Rest Ice Compression Elevation) protocol. After a few days, he noticed some bruising at the back of the leg and then contacted me to organise a ‘zoom’ remote session. After a quick chat and subjective assessment, we moved on to an objective look at the injury. I was able to instruct him to perform some movements and tests including palpating. We were very quickly able to diagnose a likely grade 2 medial hamstring tear. After this we went through the anatomy of the injury, timescales for recovery, ‘do’s and do not’s’ and then recorded a comprehensive rehab plan for the next two weeks. The whole session lasted 30 minutes and we will follow-up in two weeks to progress and get him back to full activity ASAP! Knowledge and correct diagnosis is key!
Case study 2 – A 33 year-old yoga teacher injured her shoulder two weeks prior. We had a brief telephone call to ascertain what the injury might be and it sounded like she may have injured her rotator cuff and was now suffering from a shoulder impingement syndrome. This was restricting her full range of movement and causing pain at night, sleeping in the shoulder. The main thing was that she was unable to teach fully with the pain and modify her practice. We agreed that a zoom appointment would be beneficial to confirm the injury and advise on rehabilitation. We arranged a zoom consultation the next day. Again, with the visual assessment, it was clear that it was in fact her acromio-clavicular joint (ACJ) that was strained. This changed the advice that I would have given just over the phone. We were then able to discuss the injury fully, record a comprehensive and specifically tailored exercise plan including stretches, mobility and strength work in addition to demonstrating a taping technique to offload the joint and reduce the pain. We will follow-up progress in one-week.
I hope these two examples help explain how useful a video consultation can be and can help you avoid long-term damage, reduce pain levels and get you back to what you want to do sooner!
If you want to discuss if a video appointment is right for you, please contact me directly at emerson@xphysio.com and I will be happy to email or call you back for an initial free 15 minute chat and advice.
Self-pay rates are £40 initial consultation (£30 CrossFit members) and £30 follow-up (£25 CrossFit members).
Insurance companies are now fully supporting and covering these sessions to allow your rehabilitation to start, progress and continue.
Stay indoors and stay healthy!
Emerson
CrossFit open 2018 and managing injuries…

The CrossFit open 2018 is almost upon us…
Over 500,000 people will likely participate this year and it will be a test!
Managing acute soft tissue injuries!
I suppose this is as good a time as any to talk about managing acute (and in some cases chronic) soft tissue injuries when is competition and training. As a Physiotherapist that has been involved in sport, who treats athletes of all levels and also worked in A&E for four years, I think that I am well placed to comment. Plus the fact that ‘what should I do if I injure myself?’ is probably one of the most common questions that I get asked! Depending on who you speak to you, you will probably get a number of suggestions.
Most people have heard of PRICE (Protect, Rest, Ice, Compression, Elevation) but have we moved on from this?
Let’s classify soft tissue as muscle, tendon or ligament and acute as an injury less than 48 hours old. This would include muscular back or neck pain, peripheral joint strains (ankle, knee, elbow etc), tendon (muscle-to-bone) issues (achilles, rotator cuff etc) and ligaments (bone-to-bone) such as the collateral ligaments of the knee or fingers.
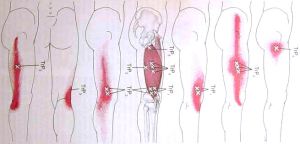
The basic healing cycle
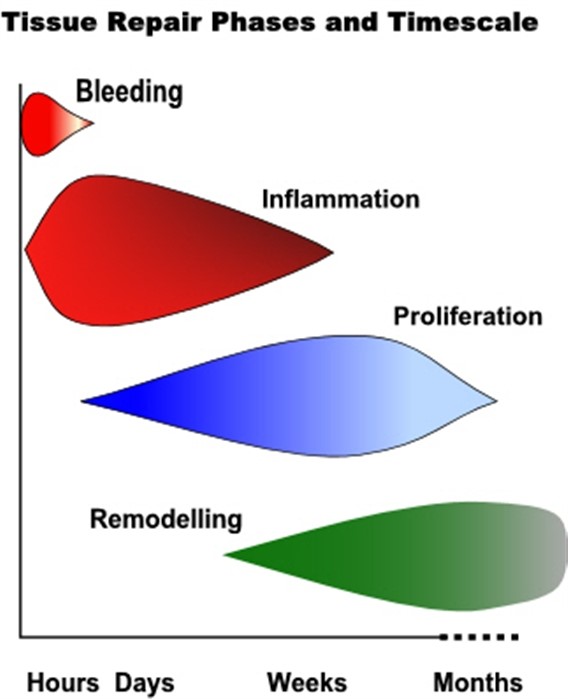
Pain relief – Paracetamol V NSAID (Non-steroidal anti-inflammatory drugs)
Concern has been raised over the use of Non-steroidal anti-inflammatory medications (NSAIDs – Ibuprofen, Naproxen, Diclofenac etc) in the early stage of injury management. This is largely due to the theory that the natural healing cycle requires the first inflammatory phase (see image below) to effectively repair injured tissue therefore trying to stop this stage too early may result in a delay overall. Evidence suggests that using NSAIDs too early (the first 24-48 hours) may compromise long-term healing. In addition, when specifically talking about muscular injuries, the early use of NSAIDs may promote increased bleeding and swelling due to decreasing platelet aggregation. This awareness of adverse thrombotic events is to be considered when weighing up risk v benefit. The use of Paracetamol as the first line of pain relief is therefore more universally accepted. It is just as effective an analgesic without the adverse effects. Obviously, you should always seek advice from your Doctor, prescribing therapist or Pharmacist before taking things especially if you have other medical issues.
Protect
Significant ligament and tendon injuries need to be immobilised. We are talking about a high-grade tear – most of the tissue is disrupted. You will know if it is a bad injury if you get immediate swelling (ie. you have fluid aggregating within a few hours), if you have a physical restriction and if you can’t bear weight on the joint. Lesser grade tears will benefit from being immobilised for a short period (48-72 hours) to prevent further damage before being re-assessed.
Rest – when and for how long?
General rule of thumb, if something is very painful and / or swollen, the body is telling you to rest. Allow the swelling and pain to reduce by offloading the structures (use a crutch, tape, support or modified position). If there is significant swelling or restriction on movement certainly 48- 72 hours is a must before you start to load the area by stretching or exercising. Look again at the stages of healing as to why this is important. Tendons take the bulk of the force whilst doing ballistic movements (running, jumping, kipping) and need ample time to recover after intense sessions and on performing new movements. Respect this.
Ice – has this treatment been debunked now?
CrossFit movement guru Kelly Starret has done a nice little discussion on topics including Ice (based around Gary Rienl’s work – links below) and really it is very similar to the discussion around the use of NSAIDs. The advice now is actually not to use ice in the initial stages of an injury however it may be more useful to use it as you start to rehabilitate. As you start to move more, we would consider any residual or further swelling to be a waste product that you want to remove. There is still a real lack of quality studies to date, particularly randomised control studies. There isn’t even a general consensus about how often and for long you ice the area for currently.
https://www.youtube.com/watch?v=0UmJVgEWZu4
I would advocate the use of heat for muscular injuries and spasm to allow the muscles to settle and allow you to start moving more quickly.
Compression
There seems to be good evidence that compression can prevent further bleeding, prevents seepage into surrounding tissue and help disperse fluid. Compression increases hydrostatic pressure and increases the effectiveness of the muscle pump, increasing venous return. Early compression is advocated in the first 72 hours, from distal to proximal in direction. Apply the compression a minimum of six inches above and below the main injury site. Do not keep compression on when lying down (sleeping)
Elevation – transient effect?
Elevation lowers capillary hydrostatic pressure (think about the effect of the body as you descend in a pool of water). Capillary flow to the soft tissues is reduced and the buil-up of edema is consequently lowered. Unfortunately, the pressures return almost immediately when the limb is returned to below heart level. Again, there is very little clinical research on elevation. I suggest in the absence of harmful effects, elevate the limb when possible and overnight.
Return to training / modifications
Once you have managed the acute first stage, pain is negligible, and you are moving the area normally it may be safe to start loading the tissue. I would suggest gentle stretching, foam rolling and tissue mobilisation with bodyweight functional movements. For example – if you have a shoulder injury, start trying to regain normal shoulder overhead movement, before trying to do a handstand or overhead press (sounds sensible huh? You’d be amazed at the amount of people that simply head back to training to test it out or just chance it hoping for the best).
If you still have some pain, take you time and train around it. If your ankle is still sore and swollen, don’t do box jump, burpees, heavy squats – choose to modify or do some upper body stuff? The coaches are the best people to talk to this about and help you scale.
When to seek advice / investigation?
If in doubt, ask. Most sports practitioners will be happy to give you five minutes of advice over email or in person. Expect minor muscular strains to improve significantly over three to four days if given the right environment to do so. Expect ligament and tendon strains to improve over three to four weeks. Expect higher grade sprain and tears to take six to eight weeks to start feeling normal again.
If you injure yourself and you cannot weight-bear, are in excruciating pain, can see that something is obviously misplaced or missing and /or if the area is hot or looks infected (you will likely feel unwell and have a temperature) then get yourself to A&E and get checked out.
If you think you have a soft tissue injury and it doesn’t improve as expected after three to four days, book in to see someone to get a proper diagnosis. Worth the money and will get you back lifting quicker and more safely in the long run. Advice on the correct management of injuries is the key to recovery!
Have a great open guys and stay injury free!
Emerson
Pec mobility drills… for everyone!
Shoulder problems?
With many injuries and restrictions I find the the pectoralis minor is often very tight and more importantly weak.
Whether this is the symptom, cause or just a secondary factor, mobilising this region is very useful.
This is a nice routine to work on the #mobility of this often tight and prohibited region.
Try:
– 10 reps arm @ 90 degrees palm up
– 10 reps @ 90 degrees palm down
– 10 reps @ 100, 110, etc Palm down depending on your restriction
– Finally you can lift the shoulder off the ground for 30 seconds to stretch out.
Test length / movement before and retest after. I like this pre and post-lifting, especially for any overhead movements #pullups #snatch #OHP # muscleups #physio #crossfit #rehab #WOD
New Canary Wharf clinic – CrossFit Thames!

Physiotherapy @ CrossFit Thames
Sunday 13/08/17
10-12 noon
Emerson (XPhysio) is a sports Physiotherapist and CrossFitter. He works regularly with weightlifters, gymnasts, athletes and weekend warriors to assist them in staying healthy and reaching their training and competitive goals.
He will be running a FREE injury clinic on Sunday 13th August between 10-12 noon. These are 20 minute appointments for injury assessment and advice. So, if you are having any aches and pains that you are not sure about, new or are simply re-occurring, then pop in for a chat! The session will consist of a movement screen with emphasis on any specific injuries with advice.
I will then be holding regular weekly clinics at CrossFit Thames – WEDNESDAY PM!
You can book in by emailing:
For information about how to book in for Physio, please speak to Coach Phil!
Free injury advice clinic 14/05/16 @ CrossFit Hackney!
Injury clinic – Saturday 14/05/16
Hi all!
I’m running a free ‘niggles’ clinic on Saturday 14th May between 9-11am. They will be approx. 20 minutes injury assessment and advice sessions. So if you are having any aches and pains that you are not sure about, new or simply niggling then pop in for a chat!

First come, first served so please contact me at emerson@xphysio.com or on 07903 247247 to book in. Open to all CrossFitters!
Momentum (CrossFit Hackney) |Arch 328 Stean Street | Hackney | E8 4ED
Thanks, Emerson (Physio)
Don’t miss out on our FREE marathon preparation evening!
Following the success of the last three years, Complete Physio is hosting its fourth annual Complimentary Marathon Preparation Evening to prepare both your body and mind for the grueling 26.2 miles.
Join Sports Physio, Chris Myers and the Complete Physio Team for an evening of marathon preparation. The evening will be packed with insight, experience and education which will aid novice runners through to regular marathon competitors.
The topics being discussed are:
- Injury prevention with physiotherapist Chris Myers
- Marathon training plans with personal trainer Ben Leach
- Optimum nutrition with sports dietitian Rick Miller
- How to train your brain for success and how to use mental rehearsals to improve performance with hypnotherapist Phil Dobson
The event is totally free and will be held on Wednesday 28th January 2015 at 6:30 p.m. on the 30th Floor of the CityPoint building.
Please click the EventBrite link to find more information and to RSVP, and we look forward to seeing you on the 28th!
http://www.eventbrite.com/e/complimentary-marathon-preparation-evening-tickets-15274201548?ref=ebtn
Best of luck with your marathon training!
Emerson
MANAGEMENT OF TENDINOPATHIES WITH ULTRASOUND TISSUE CHARACTERISATION (UTC)
Just received a really nice little article written by Jarrod Antflick and good friend and colleague Chris Myers!
They have been working with UTC and tendinopathies over the last eighteen months or so and have some really good data and thoughts on rehab now.
You can download the article for FREE at: https://zl199.infusionsoft.com/app/page/1eca04acb357e34b1aed433ba63cd590
This newer imaging technique should really make you think about the way you load tendinopathies from now on…
Consider the irritability of the tendon when designing a loading programme. 3 x 15 reps eccentric loading is not always the solution!
Consider adding in moderate and heavy isometric exercises.
Don’t forget Soleus strengthening!
Be cautious loading into end-of-range with irritable tendon or if you suspect the plantaris involvement.
Make sure you download a copy for the full read!
For more info and to book in for UTC, you can contact Chris directly: chris@complete-physio.co.uk
Cheers guys!
Emerson
Rolling, rolling, rolling… why are we foam rolling?
Keep rolling, rolling, rolling…
They are in every box, gym, yoga studio, and sports club in all shapes and sizes, textures and densities! I get a lot of questions about foam rollers!
How often? How hard? How long? Before or after exercise? Which muscles?
Chris Beardsley, a well-known sports science writer, wrote an informative article in 2013 looking at some of the evidence around foam rolling: http://www.strengthandconditioningresearch.com/2013/10/01/foam-rolling/
The article is well worth a read! It got me thinking so here is my take on things…
What tissues are we actually affecting?
Fascia – mainly. Fascia is an uninterrupted viscoelastic tissue, which forms a functional 3-dimensional collagen matrix. Basically, fascia surrounds and penetrates every structure in the body, head to toe. It is an innervated, continuous, functional organ of stability and motion. And it is tough!
What is foam rolling?
Foam rolling is a form of self-myofascial release. What is myofascial release? That is another well-debated subject! It has been suggested that applying pressures to tissues can:
1) Rehydrate tissues
2) Reduce pain (a neural response?)
3) Improve vascular function
4) Release trigger points and break up adhesions
5) Reduce the effects of DOMS (Delayed Onset Muscle Soreness
6) Improve tissue range of motion (ROM).
What is the evidence?
There is limited, good quality evidence; however, Chris Beardsley has summarised the findings so far:
1. Foam rolling may reduce arterial stiffness, improve arterial function and improve vascular endothelial function – therefore potentially increase blood flow.
2. Foam rolling may have no detrimental effects on athletic performance pre-workout – therefore no effect.
3. Foam rolling may increase joint ROM while not impeding the production of muscular force or rate of force development – pre workout mobility could increase range. It is at least as effective as static stretching however does not reduce performance which static stretching has been shown to do (http://journals.lww.com/nsca-jscr/Abstract/publishahead/Differential_effects_of_30_s_vs__60_s_static.97324.aspx)
4. Foam rolling does not acutely affect counter-movement, squat or depth jump performance. A dynamic warm-up is better.
5. There is mixed evidence on whether foam rolling increases flexibility long term.
6. Foam rolling reduces muscle soreness. A more recent study concluded that the reduced feeling of fatigue may allow participants to extend acute workout time and volume, which can lead to chronic performance enhancements (http://journals.lww.com/nsca-jscr/Abstract/2014/01000/The_Effects_of_Myofascial_Release_With_Foam.8.aspx).
When should you foam roll?
Based on the evidence and also clinical experience these are the recommendations:
– Foam roll myofascial structures to increase joint ROM pre-workout. Be specific – work on the areas that you have problems with and be specific to the exercise you are about to perform. Don’t replace a dynamic warm-up – supplement it.
– Use foam rolling post-workout for quicker short-term recovery.
– Regular use may help longer-term recovery and sustained performance.
– Make it functional – get into end of range or dynamic positions to mimic what you are going to exercise.
– It doesn’t work for everything – use other tools and types of mobility drills too!
How should I foam roll?
I work on trigger points. These have been well mapped out by Travell and Simon’s (http://www.triggerpoints.net/). Find a ‘tender’ or ‘tight’ spot, and then apply pressure with the roller for up to 20 seconds. IF it has started to ease, stay on it for another ten seconds then release. 30 seconds maximum – you don’t want an ischemic response, which will just be painful and may actually start to damage the tissue. Try to work through a few specific trigger points along the structure you are working on. Spend 60-90 seconds rolling out the area, then move on! This shouldn’t take you more than five minutes to be effective – even when looking at a large area like the lateral thigh / Illiotibial band (ITB).
I also really like it for thoracic extension – more of a joint mobilisation. Great pre-Olympic lifting and for any overhead movements where extension is key:
Other resources:
https://www.youtube.com/channel/UCnnB4zDBqZHhQ4uLTAX8eYA
http://catalysttrainingsystems.ca/2013/11/youre-not-stretching-what-you-think-youre-stretching-part-i/
http://catalysttrainingsystems.ca/2013/11/fascia-part-2/
Not a bad video demonstrating basic positions for foam rolling:
So there you have it! As always, if you have any questions please feel free to grab me or contact me!